Being in the hospital for eight days with my daughter has taught me a lot of things. I really don’t know how to begin this post, but as I write this on the sixth night of being in the hospital, I can tell you that we are ready to go home.
With Reagan’s condition, Glutaric Acidemia Type 1 (GA-1) a sickness left untreated can have devastating effects. But on the Sunday morning when this all started, Reagan woke up and we heard her cough over the monitor, a call to her Dr. was the first thing we did. She had a low grade fever and so based on these two things, her formula recipe was changed that day. An additional formula was added in and all the amounts of the other three things we mix in (Yes, her sick day formula which includes four powdered formulas) all changed.
Reagan ate well that day, napped Ok and we thought…this is not a big deal…maybe just a cough or stuffy nose, so we went on a walk. She was great! So we went on a car ride…and then it went downhill. Her temp went from 99.6 – 102 by the time we were at the ER about an hour later. B/c of Reagan’s condition, we have an emergency letter that we present to the ER in order to be seen immediately. In addition to that, Reagan’s Dr. calls ahead and lets the ER know we are coming. It’s awesome to get seen immediately, but that’s b/c it’s urgent.
The reason the hospital let us go home on Monday afternoon is b/c she ate well and didn’t have a fever and was her happy bubbly self. The scary thing though is with GA-1, you can look and act normal, but your levels inside may be off. Reagan had blood work done immediately when we arrived so we knew Reagan’s levels were OK, she also had her regularly scheduled blood work done the week prior and those results came in while she was in the hospital, so the Nemours team could look at her on the outside and know what was going on inside of her too. All of these factors combined made it seem like she was OK. Even with a diagnosis of RSV, some kids bounce back in a day, some take 3-5 days or longer. We thought maybe Reagan was one of the lucky ones and on the lesser side of the spectrum, but we were wrong.
Monday night we gave her dinner and she threw it up 20 minutes later. Getting into the early Tuesday morning hours at home, we tried a bottle at 10:30 p.m., 1:30 a.m. and 3:30 a.m. and she wouldn’t have any of it. You might be asking, why would we wake a child to feed her in the middle of the night? All I can say is it’s protocol for GA-1 patients when they are sick, her body needs more calories to work with so it doesn’t break down existing protein, like the tissue in her muscles.
Reagan’s genetic Dr. texted with me from 1:30 a.m. until Reagan refused her last bottle attempt at 3:30 a.m. She told me we needed to go back to the ER b/c Reagan wasn’t eating.
So we brought our letter, our Dr. had called the ER and told them to be expecting us. The poor guy checking people in told me to have a seat and I said, “I am not moving from this position unless it’s in THAT direction” and pointed to the ER check in behind his post and gave him a stare down that said, “watch me!” I heard someone say, “Is that Reagan’s parents? They can come back” Hallelujah!
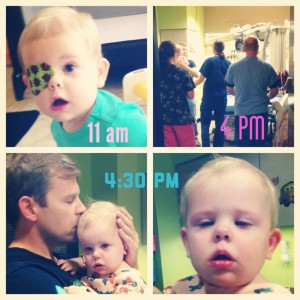
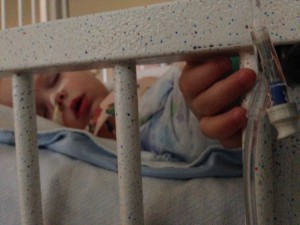
Reagan looked much more sick during round 2 at the hospital. You could just tell Reagan wasn’t feeling well, she didn’t want to keep things down, she looked sad, she had a fever and was not interested in eating a bottle. B/c of that, she had to have a tube put down her nose so that her formula could be administered that way. Over the course of two days she ripped it out three times. I couldn’t bear to be in the room when the tube was being put in…the cries she had were too heartbreaking. Instead I called my friend Rachel who’s a NICU nurse and she would calm me down, talk it out and tell me I was a good mom whether I was in there or not…Rob stayed with her, and it’s important that we know and understand where our strengths are…
Reagan got a reputation for being feisty amongst the Dr.’s and nurses on our floor. And that’s b/c Reagan is a total WARRIOR enduring IV pokes in both arms, the tube in her nose (three times) multiple blood draws and being confined to a room for a week not getting any exercise b/c you’re hooked up to tubes and IVs. And she probably thinks we’re trying to drown her in formula when she’s made it clear she doesn’t want it every time we try.
This is what is so frustrating…she needs to eat, except for the fact that she’s full of fluids and formula through the feeding tube, but we still have to try and feed her with a bottle, which she pushes away. Whatever she didn’t eat from the bottle was fed to her through her feeding tube and the never ending cycle continues. We told the nurses and Dr.’s She’s not going to meet whatever expectation you have for her to take of her formula on her own if she’s getting IV fluids pumped into her PLUS formula in the tube…AND, you’re squeezing 12 more ounces of formula than she’s used to into her body.
The never ending cycle brought me to uncontrollable crying so many times. I know how a nervous breakdown feels b/c I had one on the floor of our hospital room as Rob tried for the umpteenth time to give her a bottle. My body just shook and the tears didn’t stop and I couldn’t focus on anything and I hadn’t left the hospital grounds in a couple days and I felt the expectations being set upon us would never come to fruition and that we would live in that room.

That’s why we brought the pak and play…Oh, and we brought the high chair. We were motivated to make it normal for her so we could leave.
So I took to FB. We needed prayers…Rob and I were frustrated, Reagan was frustrated and if enduring the intensive care of a GA-1 patient during the day when they are sick wasn’t enough to make us break, the nights for Rob and I had been even worse…Rob and I would take shifts watching her to make sure she didn’t roll over, get tangled in her IVs or pull out the feeding tube in her nose.
Sometimes whoever was sleeping would be woken up as if they were shot out of a cannon by the other who was on the Reagan watch shift. One of us would scream…”I NEED HELP!!!” as Reagan would start throwing up or coughing so much that it seemed she would pass out from exhaustion. We stood over her crib for hours at a time and no one was getting good sleep. Have you ever stood in one position for four hours in the middle of the night? How about when you’re sleep deprived? Well Rob and I have, and it hurts like heck to stand that long…I started doing yoga moves to keep awake, Rob actually fell asleep standing one night and woke up to a nurse coming in to check vitals (probably should have checked Rob’s vitals too).
But there’s more…
The reason Rob and I went to Arnold Palmer is b/c it’s an in network hospital with our insurance and Nemours is out of network and the deductible is three times as high. To get the Arnold Palmer (AP) pediatrician, nurses and Dr.’s on the same page as our Nemours dietician and geneticist was a challenge. There’s two different hospitals and two different care teams. I became extremely upset at both Nemours and AP for not clearly understanding the plan at a particular moment in time. I watched as the Pediatrician spoke with the Geneticist on the phone in our room and explain a new plan before leaving the room. I explained that plan to the dietician and she was like “WHY would they do THAT?!! No No No!!! That’s not what we need to do.
I’d have detailed conversations with both Nemours and AP and try and understand and mesh what each understood from one another to see what the next steps were, and at the end of the day around day three or four in the hospital, no one who was physically caring for her at AP was completely clear on the plan. That resulted in me having a very lengthy and strongly toned conversation with both the team at AP expressing that a mistake in caring for her could have devastating effects. And I told my Nemours team I was irritated in AP’s lack of clarity on what Nemours wanted. Heck, WE didn’t even know what the goals or plan should be since we’ve never dealt with this. Which made us annoyed that we didn’t have a second letter to bring to the hospital with clearly laid out expectations or things for us and her care team to strive for. I will certainly be requesting one at the next Dr. appt. There were too many moving parts. AP was annoyed that Rob and I could have direct access to our Nemours team as we would circumvent them, but when the next feeding for Reagan is predicated on the last feeding, we only have a limited amount of time to learn and adapt at what to do next. AP could have spoken to Nemours 2 hours prior, but if we called with a new update on her feeding, it could change the diet plan instantly.
GA-1 requires intensive management, during a regular day, if Reagan doesn’t eat all of her food or formula during one feeding, it’s made up in another. We are constantly adapting her menu, it’s like hitting a moving target everyday which we have done consistently for the past 13 months, and have gotten quite good at it. So I can understand if AP is receiving orders from a Dr., they want to stick with those orders for at least a 12 hour shift but it may not be appropriate, it depends on her progress.
That hurdle was overcome…and a lot…A LOT of tears were shed as Rob and I labored in discussion for hours on how to best handle Reagan. At the end of the day, Nemours has seen Reagan since she was 7 days old. And we have cared for her since day 1. One thing we know, is we know our daughter.
On night four and during day 5 in the hospital we started to see glimpses of the corner being turned. Smiles, laughs, energy…and on Day six, she was eating her formula in 2-3 oz doses and she was crushing baby food. The Dr. at AP said if she didn’t have GA-1, she would be home…it’s the feeding and fluids we needed to see improvement on, so we were happy when we began to see that.
Friday, April 4th…my birthday started out pretty great, not only did my lovely friend Rachel have a series of gifts and cards provided for me to open every hour, she had delicious donuts delivered too. Reagan also drank three small bottles on her own and had two meals of baby food, things were looking up and all of these things were fantastic birthday presents.
But at 7 p.m. she did not want to drink her bottle so she had to have it in the feeding tube. And the nurse on that shift told us the plan was to give her 5oz every 4 hours. If you tell me she needs to have 5oz of formula every four hours (including during the night via a feeding tube, when she typically sleeps from 7 p.m. – 7 a.m.), PLUS try to give her additional bottles by mouth during the day AND meals, I can tell you her little stomach is not going to be able to do that, especially if you’re giving her fluids…she’s FULL! Try going to a brazillian steakhouse for dinner and drink a liter of water, and then do it again in four hours…and then again, and again and again. I understand giving more calories and feeding her more regularly when she’s sick is protocol. And I understand doing that through a tube when they’re sick and not willing to eat, but when she’s getting better, is drinking a little from a bottle, eating food and pulling out her feeding tube, maybe she’s trying to tell us something.
That’s when it clicked for Rob and I. We looked at each other and said, “we are never going to go home if 5 oz every 4 hours is the goal…this can not be the goal.” The nurse that came on for my birthday night shift was a Godsend as she was the first nurse who told us this was the plan that had been ordered to her…and we said, that’s nice, but this is what the plan is going to be. I spoke with the dietician and b/c she was eating and getting formula throughout the day, she was comfortable letting her sleep 6-7 hours…so we fed Reagan 5oz of her formula at midnight over the course of an hour to make sure she had enough calories in her system and planned to let her sleep until 7 a.m. In addition, at midnight the fluids were cut in 1/2 and at 4 a.m. they were cut off completely. Reagan is not going to be thirsty or hungry if she’s filled up with formula and liquid, and we need to get this baby girl home and back to her normal routine, which we have worked tirelessly on.
That worked until the Dr. came on shift and put her back on the minimum amount of fluids. We had our lengthy debrief with her at 7:30 a.m. and the phone calls and plans were made, changed, discussed, evaluated, etc. Reagan wants to eat food…she’s eating a ton of food, but her bottles are inconsistent. We feel she started to develop a bottle aversion while in the hospital b/c it was unpleasant.
Rob and I knew, drinking a bottle or two was required for us to go home and when she pushes it away, it was so frustrating. The day we were discharged, she just had to drink something…we tried so many times and finally said, you need to let us out of this room to go on a walk and try to feed it to her in a different environment. While it was a battle for her to drink it, she took 5 oz. A few minutes later we had our discharge papers and were packing up.
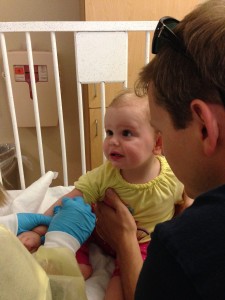
Sorry for these blurry pics, but they tell an amazing story of how much these two love each other!
Since being home, Reagan continues to eat a ton of food, pretty much her normal amount, but she still does not want that bottle. We’ve tried with a straw, sippy cup and bottle…we have no idea how we will overcome that, and are hoping that in the next day or so she will remember her routine and take a bottle. We do NOT want to go back to the hospital, we want a full recovery in all aspects and that is what we are praying for and what we are asking you to pray for.
Your prayers…they were SO needed as Rob and I were running on empty, were so exhausted and felt defeated multiple times throughout the day, so thank you SO MUCH!! Rob and I have read all the messages on FB, email, text, and listened to your voicemails…and they were so encouraging. Knowing we have so many friends and family that love us and are there for us means the world. Thank you also for offering to bring meals, and to those who helped out at our house with Bauer, cleaning, laundry…and to our friends who were our sounding boards. Coming home after 8 days was such a victory and we can’t wait to have a restful night finally. We still have work to do and patience to possess as we do it. Thank you for your continues prayers and support!








April 7th, 2014 at 12:20 pm
I just read this on the train on my way into the city, and there are tears running down my face. Incredible story of strength and love. Reagan is one lucky girl to have such amazing parents. Xo
April 7th, 2014 at 1:00 pm
You will get thru this, A-M! My oldest grandson, was a 2# preemie,born with major heart and urinary tract problems, spent his first 3 months in the NICU and had 15 surgeries by the time he was 3 years old. Well, Payton turned 10 yesterday!! And he’s a happy healthy kid! You will survive!!
April 7th, 2014 at 2:16 pm
I’m so happy The Lord has heard our cries and answered our prayers. He will continually watch over this beloved family, whom He loves and cares for so much. We give all the praise and credit to The Lord, because He carried you through this great trial. He is number 1 in your family and will sustain you always. I love my family so much and so greatful for the the prayers of family and friends.